Dry Needling
Dry Needling
You’ve most likely heard of acupuncture; and quite possibly IMS. They both fall under the category of Dry Needling. Dry needling is a technique that a trained physiotherapist can incorporate into your treatment plan. It involves the insertion of a fine solid needle through the skin barrier for therapeutic effects. The two most common types of dry needling techniques are acupuncture and intramuscular stimulation (IMS).
Acupuncture vs. Intramuscular Stimulation
The main differences between acupuncture and intramuscular stimulation (IMS) are the theories behind the treatment and the goals of treatment. Acupuncture targets many different body systems including, but not limited to, the musculoskeletal system, the digestive system, the nervous system, the cardiovascular system, and the respiratory system. On the other hand, IMS targets primarily the musculoskeletal system.
Acupuncture is based on Traditional Chinese Medicine (TCM) philosophy whereas IMS is based more so on western medicine. In TCM, pain is believed to manifest when there is a disruption of energy flow in the body. It is believed that the insertion of acupuncture needles into specific points can help restore this energy flow. Conversely in IMS, the needle is inserted into a tight and tender muscle band in order to release it. IMS has become quite popular in the last few decades and more research is coming out on its effectiveness as a therapeutic technique.
The benefits of acupuncture and IMS
Benefits of acupuncture and dry needling include reduction in pain and inflammation, acceleration in tissue healing, as well as restoration in function. According to TCM, acupuncture has also been proposed to have more holistic effects including reducing stress, improving energy and balancing the autonomic nervous system.
Common conditions that can be treated with acupuncture and IMS:
- Lower back pain
- Headache
- Rotator cuff tendinitis
- Tennis elbow
- Piriformis syndrome
- Muscle strains
How to prepare for your appointment for dry needling:
- Ensure you have eaten before your appointment.
- Let your physiotherapist know about your medical history and any medications you are currently taking. Be sure to include even over the counter medications as some have blood thinning properties.
- Let your physiotherapist know if you’ve experienced any adverse events in the past following needling.
What to expect during your appointment for dry needling:
Although we always do our best to incorporate each patient’s desired treatment, the physiotherapist will always conduct a thorough assessment to ensure you are an appropriate candidate for dry needling.
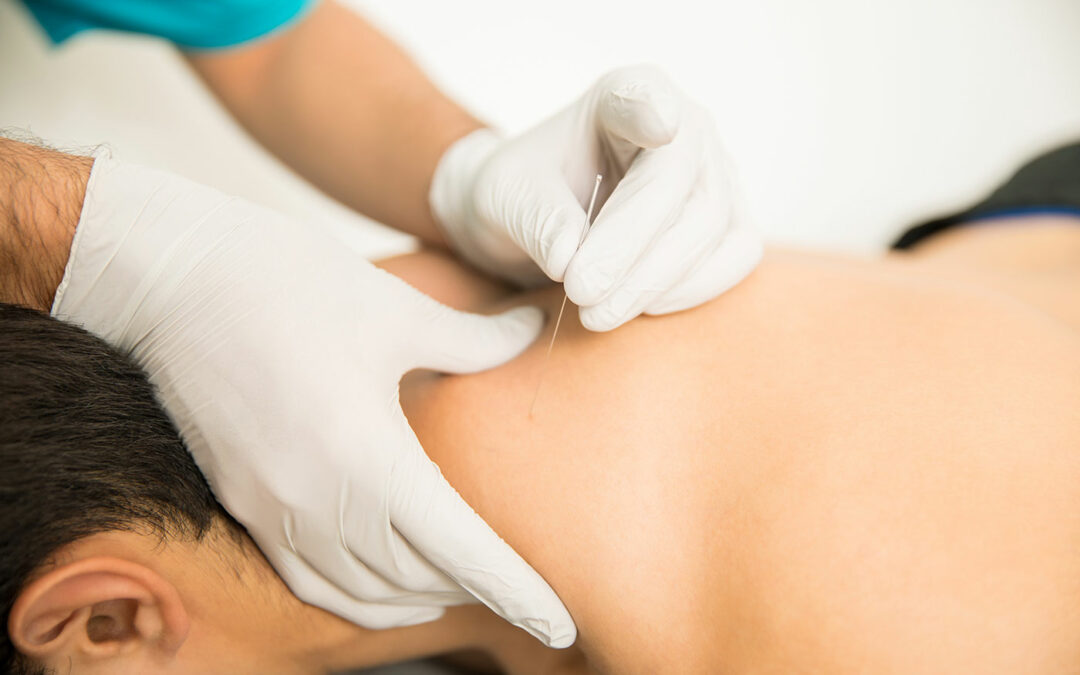
Your physiotherapist will position you appropriately for acupuncture and dry needling. Whenever possible, your physiotherapist will have you lying down for the treatment. Your physiotherapist will wear gloves for dry needling. They will also sanitize the area to be needled. You will feel a light prick when the needle is inserted. For acupuncture, once the needle has penetrated the skin barrier, you may not feel the needle anymore. For dry needling, you may experience what is known as a local twitch response during treatment. It will feel as if the muscle very briefly grasps onto the needle.
Remember that you can request to stop needling at any time.
What you Should expect after your appointment for dry needling:
It is quite common to experience minor bleeding, bruising and mild/moderate pain during or after treatment. Although there is a possibility for more serious adverse events, these are rare. Your physiotherapist will discuss these with you prior to needling. It is important to pick a physiotherapist who is well trained in dry needling as some areas, particularly those muscles located around the lung fields, can be riskier. BC requires that all physiotherapists who wish to practice dry needling have practiced for at least 2 years prior to undertaking any courses. They also approve only those educational institutions who meet their standards for safe and effective practice.
We are pleased to share that every one of our Sun City Locations has at least one physiotherapist trained and certified in dry needling. If you wish to book with one of our certified physiotherapists, please give us a call and we’ll be happy to assist you in your recovery.
Katarina Green is a registered physiotherapist who is trained in both Acupuncture and IMS.